Is Tracheostomy Permanent?
Is Tracheostomy Permanent?
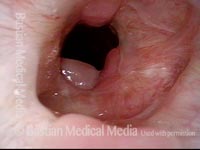
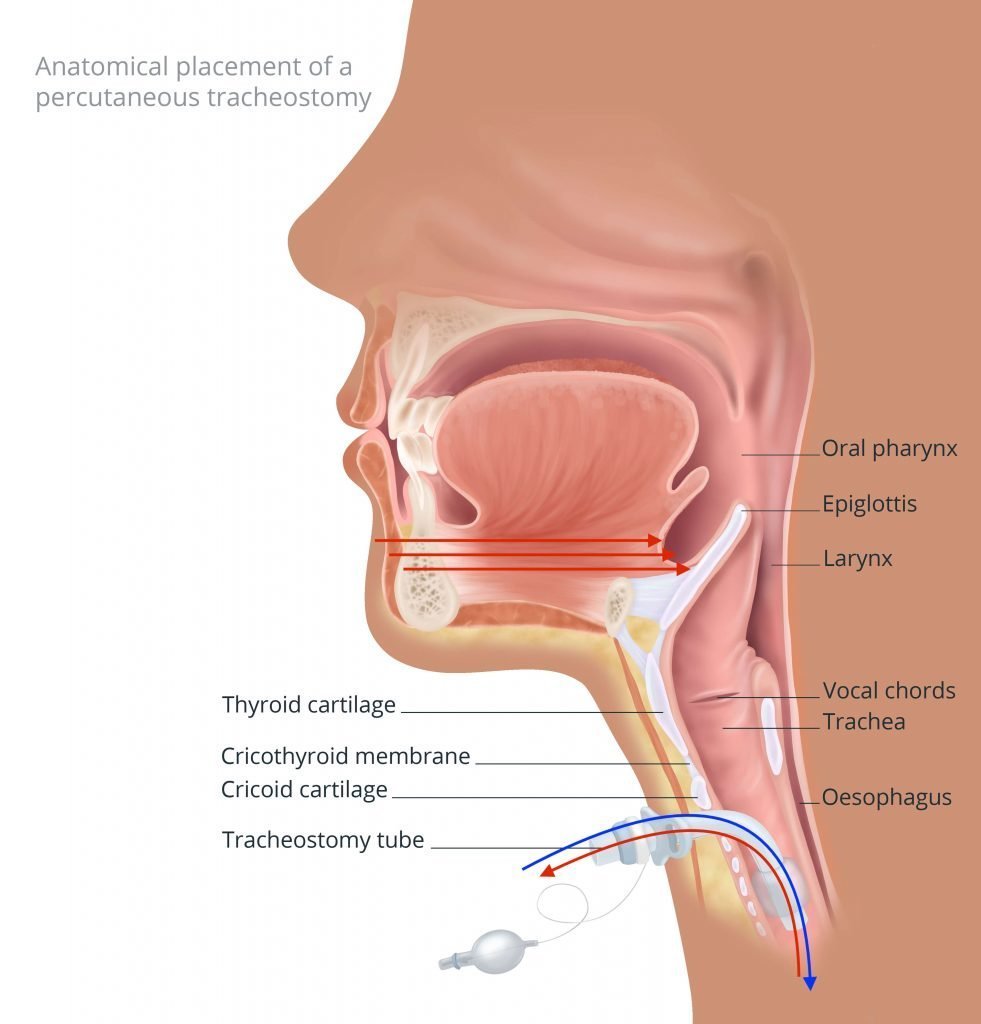
A tracheostomy is a surgical procedure to make an opening in the trachea (airway). A tracheostomy may be temporary or permanent. In most cases, a tracheostomy is intended for short term use. The amount of time a tracheostomy is in place will depend on the initial indication for the tracheostomy tube.
There are many reasons to receive a tracheostomy tube. Indications for tracheostomy include airway obstruction such as a mass or swelling. If the swelling resolves then the trach may be removed. If a mass is surgically removed or is able to reduce in size from therapies to the point where the airway is patent, then the tracheostomy may be removed. Other indications include respiratory failure due to acute disease such as pneumonia, Covid-19, or other infections. Once the infection resolves, the patient may be able to wean from the ventilator and remove the tracheostomy.
If the indication for the tracheostomy tube has been resolved, then the tracheostomy tube may be removed. However, some individuals will require the tracheostomy tube for long term or permanently if the indication for the tracheostomy tube has not been resolved.
Reasons for a permanent tracheostomy tube may include an underlying long term, progressive or permanent condition such as ALS. Other conditions are those with irreversible damage to the structure of the larynx or both recurrent laryngeal nerves, resulting in inability to breathe through the upper airway.
Other indications for permanent tracheostomy may include laryngeal paralysis or collapse and obstruction of the upper airway due to laryngeal cancer if it is unable to be removed. Permanent tracheostomy is also commonly performed in those with severe obstructive sleep apnea syndrome who are not candidates or are unable to tolerate non-invasive continuous positive airway pressure (CPAP) or surgical procedures.
The majority of tracheostomies are inserted for temporary respiratory support. If the tracheostomy was placed for an acute event, surgery or illness, the tracheostomy tube is typically removed after that initial reason has been resolved. There are some indications that indicate readiness for the tracheostomy to be removed.
When will the tracheostomy be removed?
A physician competent in tracheostomy and care is the best person to determine if the tracheostomy tube will be removed and when it will be removed. Indications the tracheostomy tube is ready to be removed include that the initial indication for the tube has been resolved, strong cough reflex, adequate swallowing, and ability to breathe through the upper airway. A child may receive a tracheostomy for undeveloped lungs or tracheal stenosis for example. If the child overcomes these issues, then the tracheostomy can be removed.
Once mechanical ventilation is no longer necessary, the literature indicates the following aspects are of particular importance to evaluate prior to decannulation:
1. Management of secretions and swallowing status
2. Airway patency of the upper airway and ability to tolerate capping
4. Level of consciousness
5. Ability to shrug in patients with cervical spinal injury.
See our section on decannulation for more information about removal of the tracheostomy tube.
After the tracheostomy tube is removed, the stoma (hole that contained the tracheostomy tube) may close immediately or typically within one week. Occasionally the stoma may need to be surgically sutured closed.
It is possible to achieve a good quality of life with a permanent tracheostomy. See communication options, swallowing management, and mobility for more information.
-

Tracheostomy Manikin
Rated 5.00 out of 5$1,895.00 Select options -

Trachie-O-Potamus Tracheostomy Unisex Hoodie
Rated 0 out of 5$29.00 – $35.00 Select options -
Sale!

Children’s Tracheostomy Book Hardcover | Trachie-O-Potamus’s Big Race
Rated 5.00 out of 5$24.99$21.99 Add to cart -

Finding Your Voice Songs for Kids with Trachs
Rated 5.00 out of 5$20.00 – $29.00 Select options