Tracheomalacia
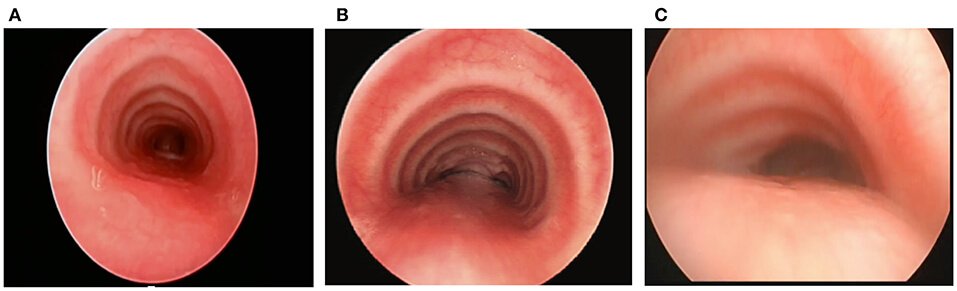
Tracheomalacia is a structural abnormality of the tracheal cartilage allowing collapse of its walls and airway obstruction. The trachea is made up of 16 to 20 U-shaped rings of hyaline cartilage, which connects the larynx to the distal airways. It is stiff and flexible, providing a conduit to carry air into and out of the lungs. A variety of different diseases can disrupt the support of the trachea, causing tracheomalacia. There are no internationally agreed classifications systems, but can be separated into congenital defects, acquired conditions and conditions causing extrinsic compression of the airway.
Congenital Tracheomalacia
Congenital tracheomalacia is more frequent in premature babies. Tracheomalacia is the most common congenital tracheal abnormality with a reported incidence of 1 in 2,100 children (Boogard, R, et al. 2005).
There is a range of nonspecific respiratory symptoms depending on the location, extent, and severity of the airway collapse. Symptoms range from mild to severe shortness of breath, expiratory stridor, barking cough, bluish skin. The airway collapse can lead to ineffective cough and reduced clearance of secretions which can result in respiratory infections, prolonged recovery from respiratory infections, and recurrent or persistent pneumonia. Cough was found in 83% of children (night-time cough 42%; productive cough 60%; exercise-induced cough 35%; characteristic barking cough 43%), recurrent lower airway infections in 63%, dyspnoea in 59%, recurrent wheeze in 49%, recurrent rattling in 48%, reduced exercise tolerance in 35%, symptoms of gastro-oesophageal reflux (GOR) in 26%, retractions in 19%, stridor in 18% and funnel chest in 10% (Wallis, C. et al 2019). In children with TM/BM, symptoms can be aggravated by any conditions requiring increased respiratory efforts, such as exercise, coughing, crying, feeding, Valsalva manoeuvres, forced expiration or lying supine. Intermittent compression of a malacic trachea during bolus progression in the oesophagus can cause desaturation, leading to poor feeding and, consequently, poor weight gain.
Tracheomalacia is associated with common systemic conditions including Ehlers Danlos and bronchopulmonary dysplasia. It is also associated with congenital diseases such as tracheoesophageal fistula and double aortic arch. These diseases weaken the trachea. Tracheomalacia is associated with laryngomalacia, bronchomalacia, tracheobronchomalacia, epiglottits, excessive dynamic airway collapse, and tracheoesophagal fistula.
Treatment for congenital tracheomalacia depends on the severity. The management of these patients is best by an interprofessional team with input from a variety of specialists. Milder forms may become asymptomatic as the diameter of the airway enlarges with the child. In some cases, treating the underlying condition can improve the symptoms. Medical management also includes ciliary clearance of secretions since the cough mechanism is impaired. Medications can be provided which minimize and thin secretions. Pulmonary hygiene is also used to help with mucociliary clearance. Controlling gastroesophageal reflux and associated aspiration is also important.
In more severe cases, more aggressive treatment may be warranted. Surgical treatment is reserved for the most severe cases, depending on the type and location of the tracheomalacia. Surgical options may include pexy procedures (such as aortopexy), silicone or long term stenting to hold the airway open, tracheal resection and end-to-end anastomosis or slide tracheoplasty. A tracheostomy may be a last resort which would allow a tracheostomy tube to be placed into the airway to provide positive pressure ventilation.
Tracheostomy and Congenital Tarcheomalacia
A tracheostomy tube may be needed for cases of severe tracheomalacia. The child now would inhale and exhale through the tracheostomy tube. Airflow would not pass through the upper airway which is the area of weakened/collapsed trachea. This can relieve symptoms of respiratory distress. The child can also be placed on mechanical ventilation if necessary. A tracheostomy for the delivery of positive pressure is reserved for more severe cases in whom other approaches have failed or where pressure support is required for most of the 24 h day.
Extrinsic Compression and Tracheomalacia
Tracheomalacia can result from extrinsic pressure on the trachea which results in degeneration of the normal cartilage. This can be caused by anatomical abnormalities such as a vascular ring, anomalous innominate artery and enlarged pulmonary veins, compression due to a mediastinal mass or tracheal weakening due to infection or prolonged tracheostomy.
Acquired Tracheomalacia
Acquired tracheomalacia develops after birth and can occur due to multiple reasons. It can also be caused by trauma to the trachea, chronic tracheal infections, or polychondritis. The most frequent cause is indwelling tracheostomy and endotracheal tube with an inflatable cuff, typically developing at the level of the cuff. Recurrent intubation and duration of intubation increase the risk. Symptoms include difficulty breathing, stridor, severe coughing fits, wheezing, recurrent pulmonary infections.
Acquired Tracheomalacia and Tracheostomy
Patients with acquired tracheomalacia may require tracheostomy to bypass the area of collapse/weakness of the trachea. However, patients with intact airways who require tracheostomy for other reasons may also develop tracheomalcia from complications of the tracheostomy tube. The local pressure effect of the cuff of the tracheostomy, particularly when overinflated, can cause inflammation, overdistension or local tissue ischemia resulting in erosion of the cartilaginous rings. It has been demonstrated in laboratory animals and autopsy material that endotracheal and tracheostomy tubes produce measurable tracheal injury during intubation periods as short as 2 hr (Ravin, et al., 1981).
Management of cuff pressures is important to prevent tracheomalacia. Cuff pressures should be monitored routinely in patients who are intubated or with tracheostomy. The frequency of cuff pressure checks is institution-specific but typically performed daily, at minimum. There are several factors that can affect cuff pressure including tracheal size, ETT/tracheostomy tube size, ventilatory pressures and patient position . The current recommendations include the utilization of a cuff pressure range between 20 and 30 cmH2O in adult patients to prevent tracheal injury (Hockey, CA et al., 2015). Over-inflation of the cuff causes tracheomalacia and can also lead to tracheoesophageal fistula, and tracheal rupture due to tracheal mucosal blood flow injury.
When tracheomalacia occurs due to an overinflated cuff, the walls protrude at the level of the cuff and become weakened. If the patient is on mechanical ventilation, there may be a persistent leak. If more air is placed into the cuff to achieve a seal, this can then further damage the tracheal wall. If diagnosis is confirmed for tracheomalacia, the tracheostomy may be changed to a longer tracheostomy tube to bypass the level of tracheal wall damage and create an optimal seal. Placement of a double cuff tracheostomy tube is another option. Other options include stenting, trachoplasty, tracheal resection, tracheal dilatation with surgical stent placement, t-tube placement, tracheal replacement, or surgical attachment of a polyethylene or polypropylene mesh onto the trachea at the area of the malacia.
Diagnosis of tracheomalacia

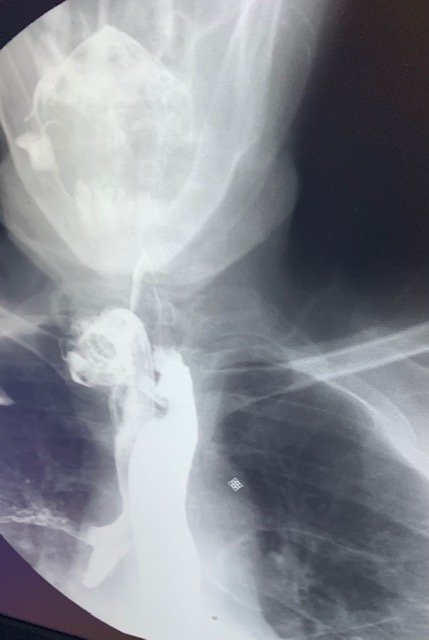
Diagnosis of tracheomalacia is typically made by bronchoscopy, which is the gold standard. Bronchoscopy has the advantage of being able to assess the airway dynamically during all phases of respiration. Chest x-ray, computed tomography angiography (CTA), magnetic resonance imaging (MRI) and echocardiogram, as well as fluoroscopy, and/on tracheography with contrast agents may provide additional information. During forced expiration and/on cough, the increase in intrathoracic pressure causes collapse of the trachea wails. Pulmonary function testing can be helpful which shows a characteristic reduction in peak expiratory flow.
Other Classifications of Tracheomalacia
Tracheomalacia can also be classified into posterior intrusion, anterior collapse, or vascular compression. Check out the video below from Boston Children’s for a great review of this information.
Summary
Tracheomalacia is a clinically challenging condition and interprofessional management is often required to optimize the management of the disease . It may be congenital or acquired. A tracheostomy tube may be required in severe cases as a last resort where other approaches failed or where positive pressure is required. Tracheomalacia can also be caused by overinflation of the cuff of a tracheostomy tube. Cuff management is imperative to prevent tracheomalacia.
Related Webinars
Resources:
Hockey CA, van Zundert AA, Paratz JD. Does objective measurement of tracheal tube cuff pressures minimise adverse effects and maintain accurate cuff pressures? A systematic review and meta-analysis. Anaesth Intensive Care. 2016 Sep;44(5):560-70. doi: 10.1177/0310057X1604400503. PMID: 27608338.
Ravin, C., Handel, D. & Kaniman, K. (1981). Persistent Endotracheal Tube Cuff Overdistension: A Sign
of Tracheomalacia. American Journal of Roegenology.
Wallace, C., Alexopoulou, E, L. Antón-Pacheco, J, Bhatt, J. M.(2019). ERS statement on tracheomalacia and bronchomalacia in children. European Respiratory Journal. https://erj.ersjournals.com/content/54/3/1900382








Responses